When Dr. Alireza Maghsoudi graduated from his residency at Georgetown University Medical School in 2002, he had never had so much as a lecture on the health benefits of sleep.
“Historically, sleep has not been a subject that doctors thought was important,” says Maghsoudi, an attending cardiologist at Virginia Heart.
That’s changed on both sides of the doctor’s office: Physicians are reporting that more patients are coming in with concerns about sleep problems, and as researchers find more connections between sleep and a variety of health conditions, practitioners in many specialties are asking about sleep patterns when looking for the keys to help patients get a handle on their health.
“Now we actually have a field of sleep medicine,” Maghsoudi says. “People actually do fellowships in sleep medicine, and there’s a board certification in sleep medicine. It’s interesting how the whole field has been completely changed.”
“We see sleep as an integral component to how we function in terms of day to day,” says Dr. Erica Martin Richards, the chair and medical director for the Department of Psychiatry at Sibley Memorial Hospital. “Everything that we do is so dependent on sleep.”

How Much Sleep?
In general, we don’t live lifestyles that are conducive to sleep.
“We live in America,” says Dr. Amit Patel, medical director of the Sleep Center at Virginia Heart. “We’re very capable, active go-getters; we’re very productive. And so, in our society, we value sleep less in my opinion than we should, because we like to be productive. … But, although we get short-term benefits for getting more work done, the long-term detriments of lack of sleep are pretty profound.”
The National Sleep Foundation recommends most adults try to get seven to nine hours of sleep a night. Maghsoudi agrees but says that older adults tend to need a bit less sleep, so if someone is getting six hours a night and can’t get a seventh, it’s not worth prescribing a medication that could have various side effects.
Richards points out that there are two main types of sleeping problems: getting to sleep and staying asleep. The former is often a matter of sleep hygiene — the routine that people follow before getting into bed.
All the doctors agreed on a few simple steps to help fall asleep faster. Keep a consistent bedtime; put down the electronics for at least a half-hour (preferably an hour) before you hit the sack; and don’t spend time in bed making phone calls, reading, or scrolling through your phone.
Many people take melatonin, convinced that it helps them get to sleep. Maghsoudi describes himself as “a believer” in the effectiveness of melatonin but says there’s not convincing scientific data to back that up. Still, melatonin has no harmful side effects, he says, so he labels it “definitely worth a try.”
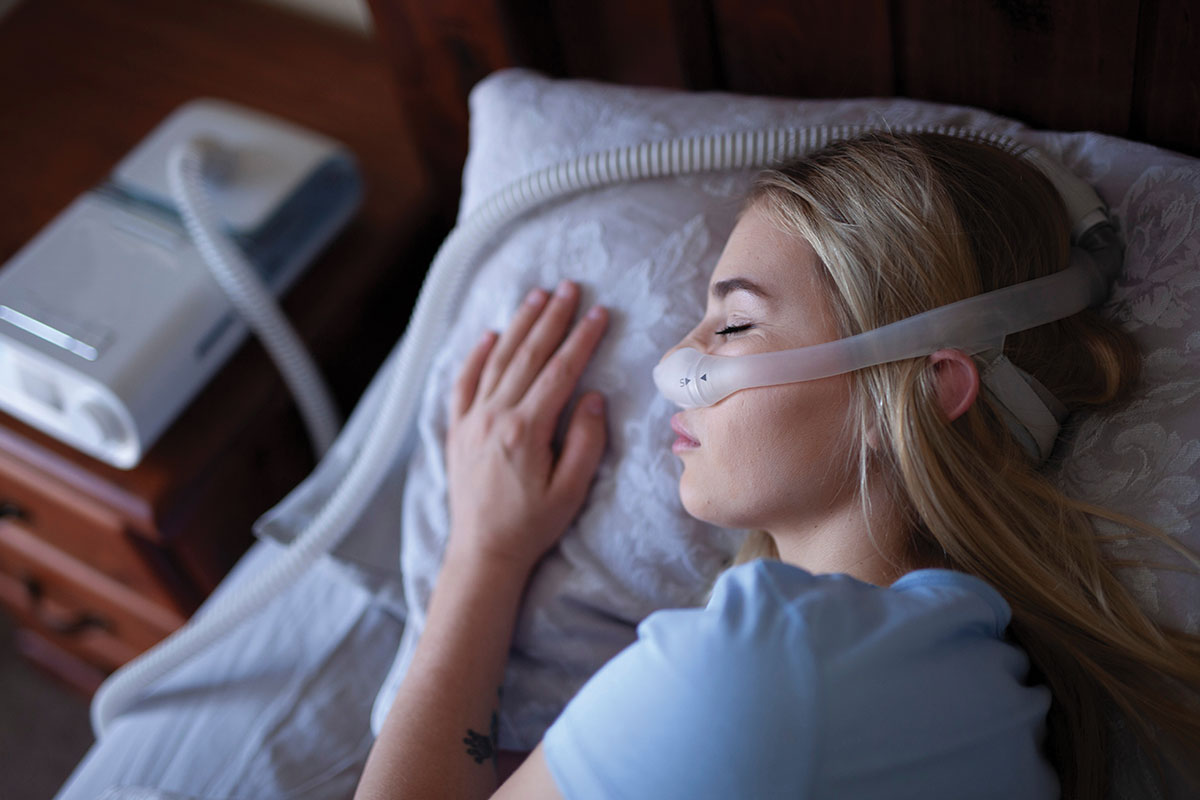
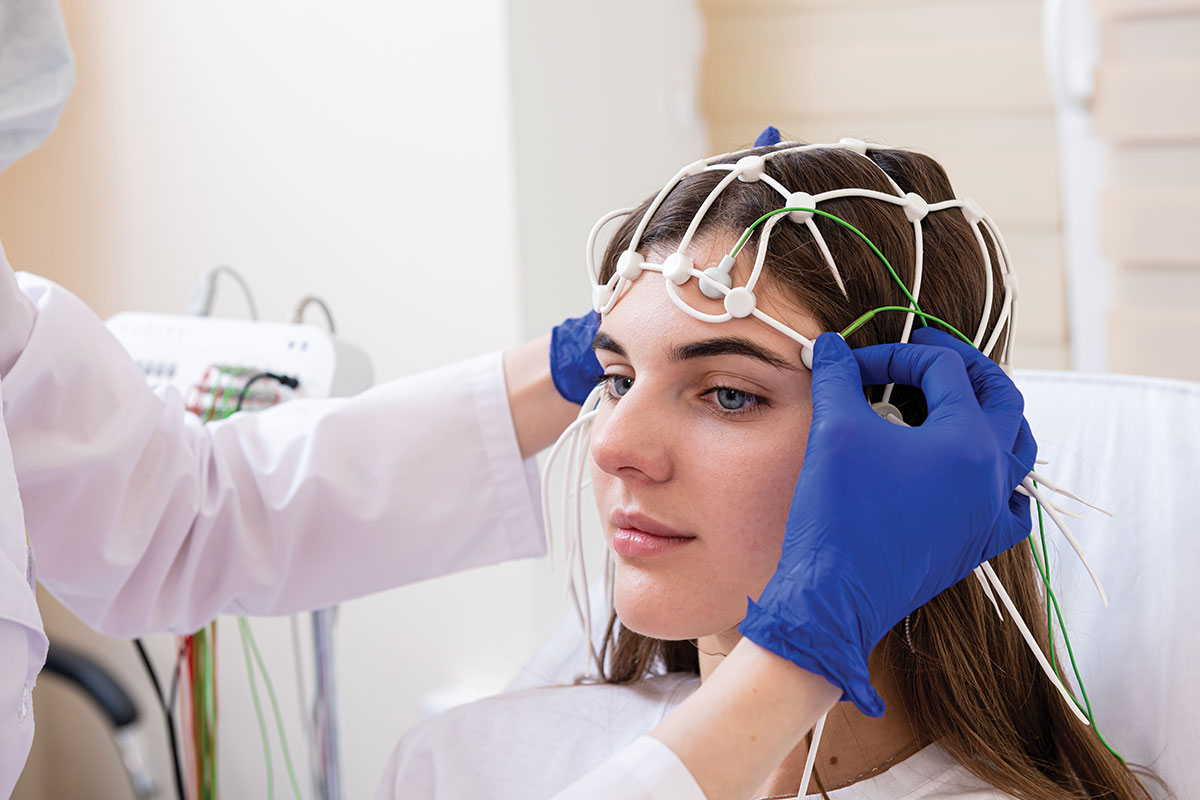
Trouble staying asleep often means patients will wake up feeling more tired than they were when they went to bed. If that’s the case, Richards says, she’ll ask a patient to undergo a sleep study, which often leads to a diagnosis of sleep apnea — a closing of the air canal during sleep, often accompanied by snoring.
“Sleep apnea increases risk of many cardiovascular conditions,” Maghsoudi says, such as hypertension, stroke, arrhythmias, congestive heart failure, and more. “So as a cardiologist, we really try to be the first to pick up somebody who has obstructive sleep apnea. There’s a lot of papers written that [say] cardiologists should really have a low threshold for treating sleep apnea, because it really makes a big difference.”
He adds, “Always ask your partner ‘Hey, do I snore? Do I stop breathing in middle of the night?’”
Making It a Priority
It’s easy to just say that not getting enough sleep can make you grouchy, but Richards says that fatigue can take on the symptoms of other psychiatric problems.
She says sleep is one of the first things she asks new patients about. “If they’re not sleeping, that’s typically the first thing that I want to target. … Without sleep, we truly sometimes don’t know if there’s a secondary underlying cause, or if someone has anxiety or increased stress or depression simply because they’re not getting consistent restorative sleep on a regular basis.”
Dr. Tyish Sonteem Hall Brown, director of behavioral sleep medicine at Children’s National Hospital, says a lack of sleep can affect kids in school in many ways, from difficulty paying attention to a lack of emotional control to decreased performance in after-school activities such as sports.
She says she talks with teens about prioritizing sleep. “Even though that sounds like a really easy fix, when we start to think of something as our priority, we find a way to make it happen.”
She sits down with teenagers and examines their schedules, centering the proper number of hours as the priority. “We say ‘OK, we know we need this amount of sleep, and we know you have to wake up at this time to go to school. So, what can we do to make that happen?’”
Solutions can include reducing “procrastination time,” reducing the overlap of extracurricular activities, and postponing social interactions until the weekend. And most of these techniques work for adults as well.
It’s about “how to adjust our schedules and really maximize the time we have, but to prioritize sleep within that scheduling process,” she says.
Physical Effects
It’s not just about mood and psychiatric problems either. Lack of sleep can contribute to a number of ailments that used to be considered unrelated.
The World Health Organization announced years ago that night-shift work, with its attendant lack of sleep, was a probable carcinogen.
“People who don’t sleep enough, their body is under a continuous amount of stress,” Maghsoudi says. “And all these stress hormones, they can actually have bad effects on the immune system,” which is designed to fight off the genetic mutations that are key to most cancers. Chronic sleep problems should be thought of as similar to pollution or poor diet, in terms of increased risk of cancer.
Patel points out that without enough sleep, “it’s almost like you’re in a constant fight or flight.” When that happens, “your body’s not sure what’s going on” and isn’t able to recycle the hormones that fight inflammation. And doctors and researchers worldwide are connecting inflammation with a growing list of health problems, including heart attacks, strokes, diabetes, and obesity.
“When you’re not getting enough sleep,” Patel says, “you’re essentially inflaming the body and you’re stressing a lot of the body’s systems.”
The Good News
Patel likes to look at things the other way around. “If you’re not getting enough sleep, there’s very good data that shows that just by getting more sleep, you can actually lose weight, without anything else.”
And Maghsoudi, who never had a sleep lecture in school, now has a whole sleep practice and sees other branches of medicine waking up to the importance of sleep.
“A lot of other specialties now are saying, ‘Hmm, I’m having trouble controlling this person’s blood sugars. Maybe it’s a sleep problem.’ … The data is suggesting that improving sleep — quality, quantity, you name it — actually helps other outcomes, and it kind of works in conjunction with a lot of other treatments.”
Feature image, stock.adobe.com
This story originally ran in our February issue. For more stories like this, subscribe to Northern Virginia Magazine.





