Amy Gillis, MD, is a board-certified radiation oncologist with the Mid-Atlantic Permanente Medical Group. She sees patients at Kaiser Permanente medical centers throughout Maryland.
If you find yourself staying up at night worried about getting a mammogram, know you are not alone. For many women, the anxiety around an uncomfortable screening or the possibility of getting abnormal results may be significant enough to skip mammograms.
In fact, data from the Centers for Disease Control and Prevention reveals that one-third of women aged 40 and up did not have a mammogram within the past two years. And a national survey showed that an alarming 22 percent of women aged 35 to 44 never plan to undergo one.
As a radiation oncologist, I understand the apprehension surrounding mammograms. Yet, I have seen firsthand how early detection saves lives. I want every woman to understand that a mammogram is an opportunity to catch an illness and provide the best shot at successful treatment.
One in Eight Women End Up with Breast Cancer
Breast cancer’s prevalence is undeniable. Among all U.S. women, breast cancer is the second most common cancer and the second most common cause of cancer death. About one in eight women will be diagnosed in their lifetime. For Black women, the risk is even higher before the age of 40 than their white counterparts.
Yet, hope shines through the statistics. Early detection transforms breast cancer into a highly treatable condition. For example, the five-year survival rate for localized breast cancer — meaning the cancer has not spread outside the breast — is 99 percent. Compare that with a 30 percent five-year survival rate once the cancer has spread to distant parts of the body. That is why we need to catch breast cancer early — and why mammograms are so important.
I encourage women to arm themselves with information about the screening process, and initiate conversations with their healthcare providers to ensure lifesaving screenings are not missed.
When to Get a Mammogram
The optimal time to start getting mammograms, and how often you should get them, is a personal choice and one that should be made with your physician or healthcare provider. Timing may depend on whether you have a personal or family history of breast cancer. This year, the U.S. Preventive Services Task Force drafted recommendations to begin biennial screenings at age 40, instead of 50, given the benefits of early diagnosis.
At Kaiser Permanente, we’ve already implemented screenings for average-risk women as early as 40. What we see in our data is that this screening saves lives. Our patients have a 41 percent lower mortality rate from breast cancer than the national average.
What to Know About Mammograms
Many women dread mammograms because they are uncomfortable.
While the compression between the two mammography X-ray plates may cause brief discomfort, most patients find it tolerable. To enhance your comfort during the process, have open conversations with your healthcare provider to address concerns and gain confidence about the process.
I recommend women choose appointments early in the day due to the need for clean, deodorant-free skin. Avoid scheduling a mammogram for the week preceding or during your period to minimize breast sensitivity.
The process is less stressful when you’re prepared. On the screening day, bring your prescribing doctor’s contact details, relevant medical history, and prior mammogram information. At Kaiser Permanente this information is stored in a patient’s electronic medical record so there’s no need to bring anything. Don’t use deodorant, lotion, powder, or perfumes, as they may interfere with the image. Wear an easily removable top and remove all jewelry. Be ready to discuss any changes in your breasts with the technologist.
For added comfort, some patients find avoiding foods and drinks with caffeine five to seven days before the exam helpful.
Today’s mammogram technology has evolved, enhancing accuracy and efficiency. Digital mammography leads to faster image acquisition. Detection rates are improved with 3D mammography. Contrast-enhanced mammography highlights abnormalities. All of these advancements redefine the landscape of breast health. Some high-risk individuals can benefit from breast MRIs and ultrasound- guided biopsies.
Worrying about radiation is normal, but the mammography’s radiation dosage is very low. And the benefits of early cancer detection far outweigh the minimal radiation exposure during mammograms.
Waiting for results can be agonizing. That’s why at Kaiser Permanente, we prioritize patients receiving their mammogram results in 30 minutes or less. We want to avoid sleepless nights for waiting women and their families.
It is common for patients to get called back after a screening mammogram because a radiologist may see an abnormality on the breast image. Of course, this can be scary. A patient who is called back may need a diagnostic mammogram, a biopsy, a breast ultrasound, or several of these. If you are called back, you may want emotional support from family or friends. Since the call back process can be unnerving, we strive at Kaiser Permanente to make the entire process as quick as possible from diagnostic test to results.
In roughly 90 percent of cases, findings turn out benign. For those needing treatment, Kaiser Permanente stands by you with expert guidance and medical care throughout the process.
Don’t postpone your mammogram. For National Breast Cancer Awareness Month, you can overcome the fear of getting a mammogram and take meaningful steps to stop breast cancer. Remember, you are not alone, and your commitment to breast health is a powerful step toward a healthier future.
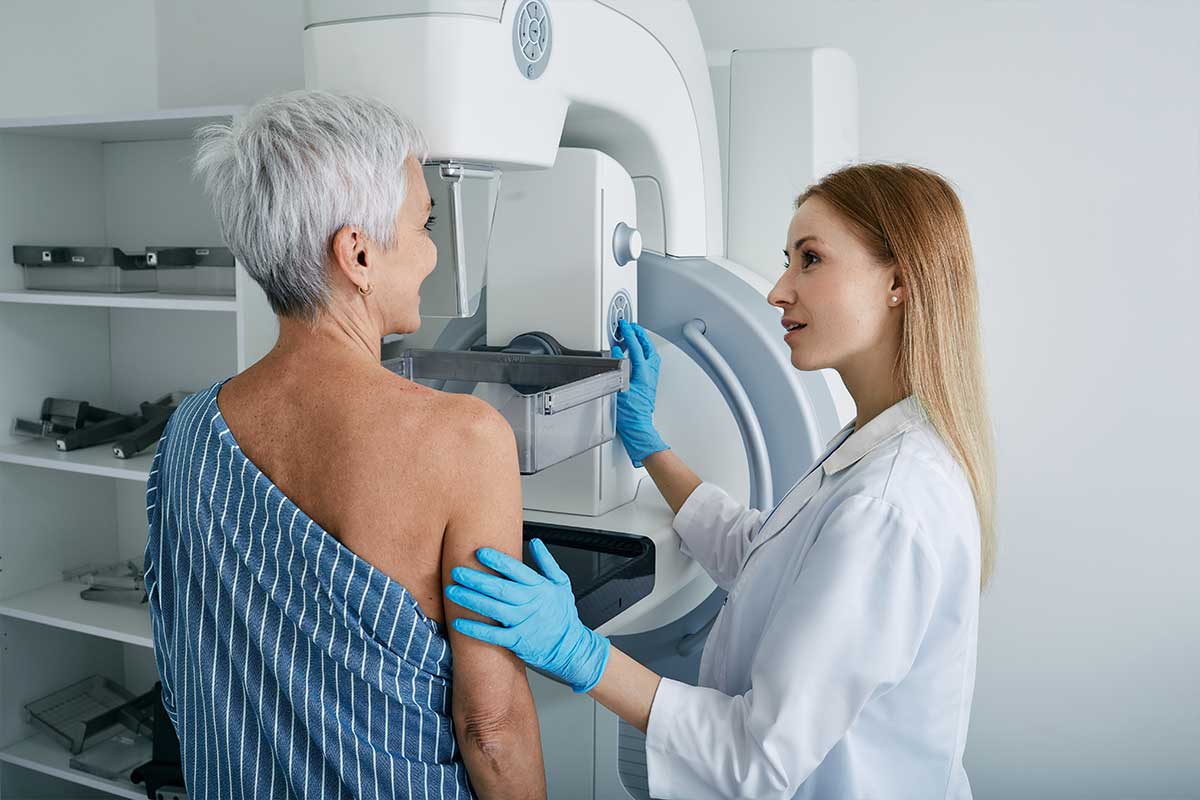
Feature image by Peakstock/stock.adobe.com
For more expert advice, subscribe to Northern Virginia Magazine’s Health newsletter.