Nearly a year into a devastating pandemic, doctors have played a central role in helping humanity fight a virus and offering us all a bit of hope. But what gives them hope? It turns out, oftentimes it’s their own patients. This year, we asked local doctors to tell us a story about a patient that has stuck with them over the years. Whether it’s a patient in recent memory or someone from decades ago, these uplifting stories remind us that there are heroes among us.

Dr. Curtiland Deville Jr.
Radiation Oncology, Johns Hopkins Sidney Kimmel Comprehensive Cancer Center, Sibley Memorial Hospital
Growing up, I always knew that I wanted to be a doctor. Since no one in my family was a doctor, when people would ask what kind, I would say pediatrician and later sports medicine, presumably because that’s all I knew. However, when I started my third-year clinical rotations as a medical student, I was immediately drawn to oncology when I experienced patients receiving a life-changing diagnosis in a moment. I had a strong desire to support them through their journey of understanding, workup, treatment and management. I became fascinated with radiation oncology and the opportunity to use ever-changing and evolving technology to target, treat and potentially cure cancer, often with completely noninvasive techniques. During my residency training in radiation oncology, I was drawn to prostate cancer when I noticed men—from stoic to chatty to everything in between—being diagnosed and needing to navigate complex treatment options during potentially sensitive and uncomfortable conversations regarding topics like erectile, bladder, bowel and sexual function in addition to survival and prognosis.
Because prostate cancer is the most common cancer in men, I see men from all walks of life, and I ultimately have the same goals of care to achieve. One very satisfying patient scenario was recently supporting a patient who was diagnosed simultaneously with a muscle invasive bladder cancer and oligometastatic prostate cancer. He is a yoga instructor and scuba diver, so the surgical option of removing the bladder and prostate that was presented to him at an outside institution was not easily compatible with his lifestyle and the activities that he enjoyed in his retirement. He sought a second opinion at our institution, and after multidisciplinary review of his case, we offered him a trimodality strategy known as bladder preservation, where he underwent resection of the bladder tumor followed by concurrent chemotherapy and radiation. He remained without evidence of bladder cancer and was able to resume the activities that brought him great pleasure. It was extremely pleasing to review his pictures from Bali, where he continued his yoga and scuba diving.
When cancer touched my family, I found that to be my most stirring patient scenario. I was there to support my close uncle when he was diagnosed with metastatic prostate cancer and ultimately passed from it three years later. Prior to then, prostate cancer management was somewhat abstract. I could think about things in a somewhat dissociated, intellectual and very clinical way. With my uncle, I had to still do that, but I was forced to understand the emotional toll and impact of every decision, every new piece of information, diagnosis, blood test and imaging result, the periods of uncertainty and the unknowing of exactly how things would play out, despite knowing all of the statistics on outcomes and prognosis. I can only imagine that this duality was meant to make me a more compassionate and empathetic doctor, as scarring and jarring as it was. Because of that experience, I can sit with my patients, particularly those who are not curable, and acknowledge the depth and breadth of their emotions in an authentic way. Although I still mourn the loss of my uncle, I am thankful for those life lessons.
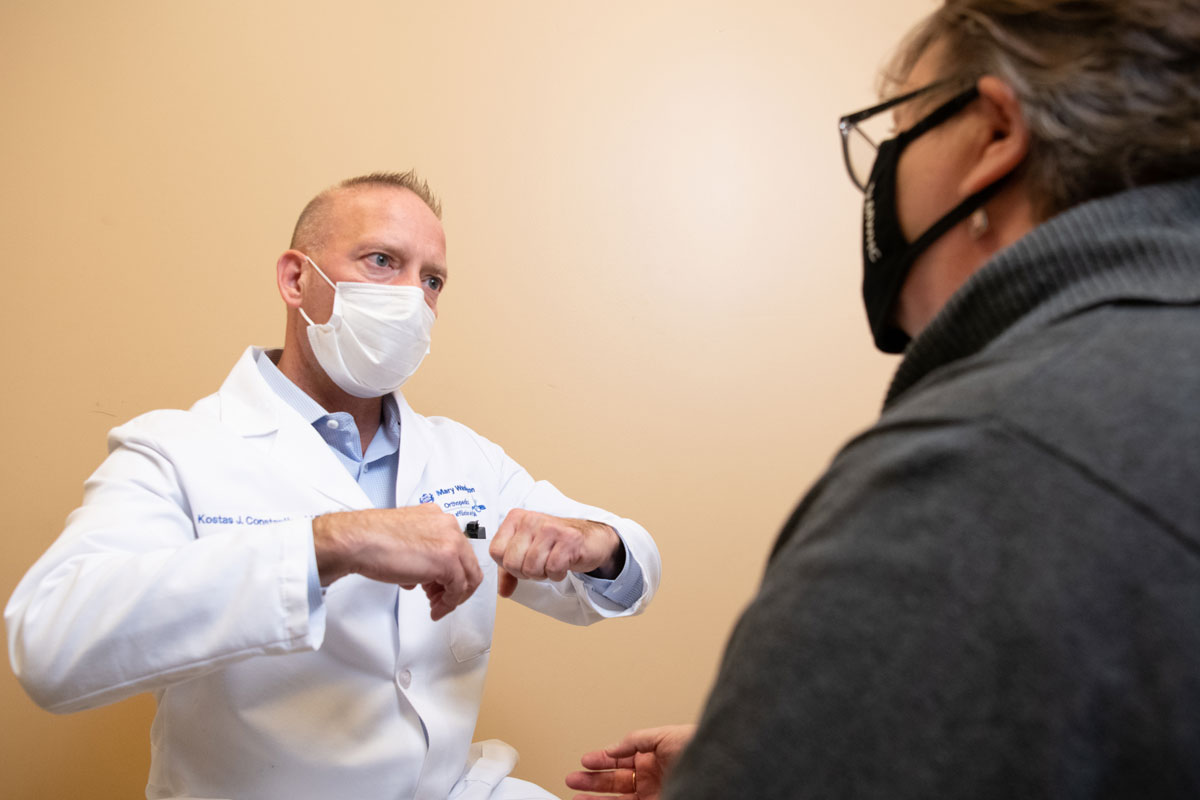
Dr. Kostas J. Constantine
Orthopedic Surgery, Mary Washington Healthcare
One day in the fall of 2003, I received an urgent request to assist one of my orthopedic partners in the operating room. I left my clinic and rushed to the OR. My associate quickly explained to me that the patient was an 8-year-old girl who had recently fallen; she presented with a severe open fracture of her elbow and forearm that he had operated on the day before. The astute floor nurses were concerned about her severe pain and asked him to reevaluate her. He immediately called the OR staff, who urgently readied a room, and she was now on the table. He needed assistance when he found that she had a severe infection with nerve and muscle damage in her forearm. The patient required six more surgeries to clear the severe infection and finally allow her bones to heal. Her parents were extremely attentive and supportive as I explained to them I thought she would have long-term dysfunction of her hand.
Neither she nor her family were deterred by my pessimism. She went through intensive therapy and worked diligently to regain some of her hand function. She even began to play the violin. As she grew, however, she developed some more long-term symptoms that affected her hand function and required several more operations over the next 10 years. During that time, however, I was able to watch her blossom: learning to play the drums in the band, getting a puppy, visiting Disney, attending college for special education, going to Owl City concerts, getting married and now expecting! Even with such a severe injury as a child, she persevered.
Her story reminds me of what being a physician is all about. To help take care of people under difficult circumstances and then see them recover and succeed is what makes our work as physicians so satisfying. I always try my best, and I only regret that surgery is not always 100% successful no matter how hard I work.

Dr. Rebecca E. Levorson
Infectious Disease, Pediatric Specialists of Virginia
As we have all endured the COVID-19 pandemic, we have faced situations never encountered before, which have required flexibility and teamwork. So I want to share a topical story related to this.
On one Saturday evening in May, when most people were finishing dinner or starting to watch a movie at home, I received a call from a colleague in the emergency department. My colleague was evaluating an ill child with COVID-19 who would be hospitalized. My colleague wanted to know what else could be given to the patient to prevent further worsening of the patient’s respiratory illness. After hearing about this patient, I dropped what I was doing and headed straight to the emergency department to see the patient. Specifically, I needed to determine if the patient would qualify for administration of the antiviral medication remdesivir, which was still an experimental treatment at that time.
The patient’s illness was severe enough that he did qualify for remdesivir, but there were many more steps needed before he could receive the medicine. Time was of the essence for this patient as his breathing could have significantly worsened the longer his illness lasted, and waiting until Monday to approve remdesivir was not acceptable. So I called my research coordinator to get remdesivir approved on a Saturday evening, and she made it happen. The hospital pharmacist was able to then measure the correct amount for the patient, and his nurse gave the first dose without any problems. Over the next few days, the patient continued to receive further doses with gradual improvement in his breathing. Before our eyes, we saw the treatment helping the patient. Eventually, the patient was able to leave the hospital.
This story highlights the power of cooperation and teamwork for our patients. I have never felt so lucky to be able to work collaboratively with so many people as I have during the COVID-19 pandemic. Each health care member has an important role to play in the care of our patients, and I embrace these collaborations, which have been born out during a very challenging time.

Dr. Ara M. Maranian
Cardiovascular Disease, Novant Health UVA Health System
Over the course of my career—both as a civilian doctor and as an Air Force major serving two tours in Iraq—I’ve had many impactful patient experiences that have taught me valuable life lessons.
One patient who sticks with me to this day was someone I saw before I was even a practicing physician. I was on my very first clinical rotation—general surgery at the VA Medical Center in Washington, DC—and an older gentleman was admitted toward the end of his life presenting with an untreatable cancer.
As a third-year medical student, I didn’t make any decisions or provide any specific treatment. The only care I was responsible for was rounding on him daily and checking on him throughout the day. He told me stories of his life, and we had conversations about current events, but I didn’t really do anything to relieve his physical pain. When he was discharged, he left a handwritten card for me at the nurses’ station, thanking me for all the great care I had provided.
It caught me off guard; I didn’t think I’d had a direct effect on his care since I didn’t perform any procedures or make any decisions. By simply visiting him every morning and spending quality time with him, it hit me that I did have an impact on his care. I didn’t realize it at the time, but those conversations about his life helped take his mind off his prognosis. Though I didn’t think much of our talks, our daily encounters gave him something to look forward to while he was in the hospital.
He passed about a week later in his home, but I still hold on to his card to remind me that medicine is about not just the diagnosis but also our interactions with a patient. As a doctor, these one-on-one conversations can influence patients in ways we might not realize. We don’t often see the significant impact our actions have on our patients, most of whom are faced with scary circumstances that may leave them feeling vulnerable.
I often find myself thinking back to my time with this patient, and it makes me smile to remember the impact he had on me, as well. Though a card may not seem like much to most, through it, he taught me to be deliberate in every interaction I have with someone, in medicine and in life.
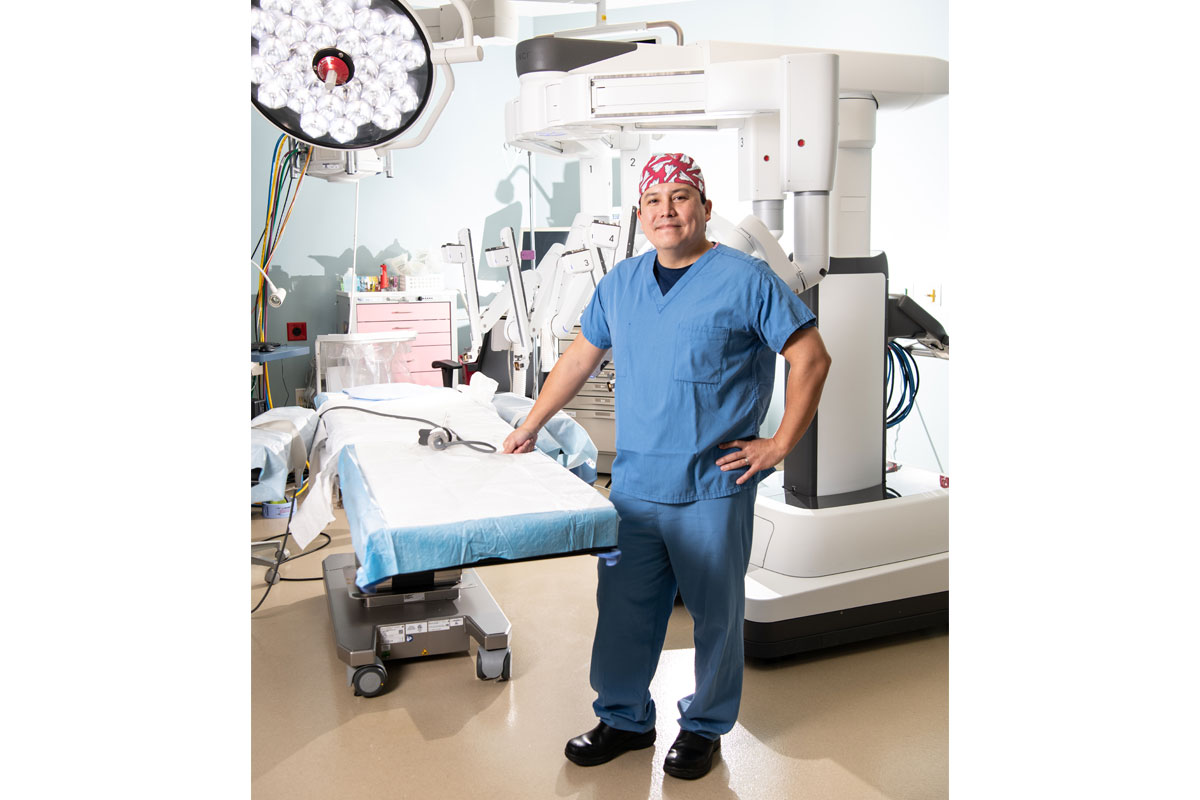
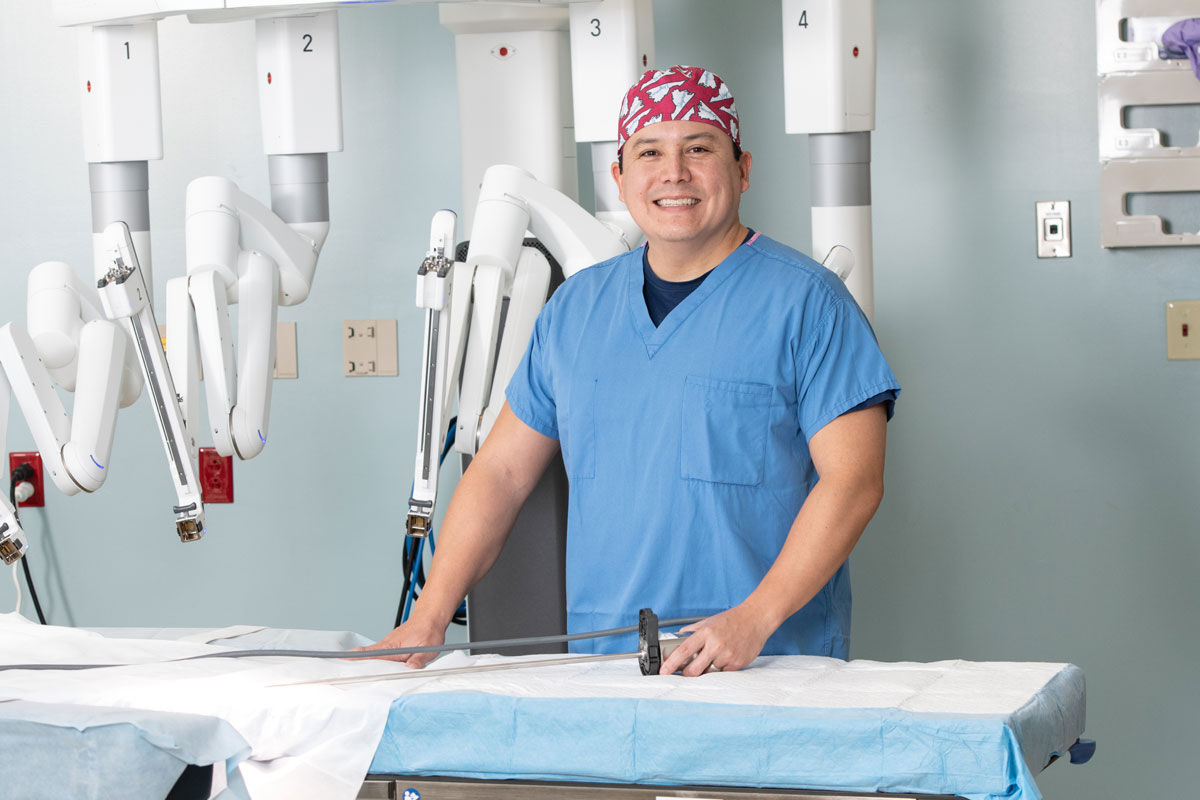
Dr. Steven K. Nakao
Surgery, Sentara
No one wants to hear they have cancer. From personal experience, I know that there is a lot of fear, sadness, anger and hope when dealing with such a diagnosis. When you have a newly diagnosed cancer complicated by the COVID pandemic, all of those emotions are amplified. Recently, I had the opportunity to treat someone who was experiencing abdominal pain and bleeding for months. Like many of us, the patient tried to rationalize it as something else. Unfortunately, like many other patients this year, she was not able to have the necessary tests to work up her symptoms due to the fear of and restrictions from COVID. When she was able to get evaluated, she was found to have a large ulcerating colon cancer. At that point, we tried to expedite and coordinate medical and surgical care for her newly diagnosed colon cancer.
After reviewing her records and discussing options, I recommended a robotic colectomy would be best for her. At a time when hospitals were not doing elective surgery cases, we proceeded with the surgery as soon as possible, understanding that this was not an elective surgery. Unfortunately, as I sent her for preoperative testing, we quickly learned she was positive for COVID, which made for a very difficult phone call prior to her surgery. Once again, we were faced with another delay. Unsure of how severe her COVID symptoms would become, we postponed the surgery for two weeks out of an abundance of caution for her and the staff.
Fortunately, her COVID symptoms were mild, and we proceeded with surgery at the next scheduled date. Her surgery was uneventful and went exactly as planned. Since we were able to perform a robotic colectomy, she had minimal postoperative pain, she regained her strength quickly, and she was discharged from the hospital in two days without any narcotics. Most importantly, regardless of all of the delays, she had a very favorable pathology and had a stage I colon cancer. During her follow-up appointments, she was told that she would not need any further treatment for her cancer and would only need surveillance for now.
I was so fortunate to be part of the team for her care. I am thankful to be able to offer patients the best in surgical care as we continue to strive to improve health every day.

Dr. Patricia Rodriguez
Medical Oncology, Virginia Cancer Specialists
About 10 years ago, a woman in her 70s with multiple myeloma came to see me for a follow-up after her regular oncologist retired. I was immediately struck by the patient’s positive attitude and unwavering smile. As we discussed her past treatment for multiple myeloma, she mentioned that she’d previously had breast cancer when she was in her 40s.
As the physician in charge of genetic testing at Virginia Cancer Specialists, I’m very interested in patient histories. I was immediately concerned and asked her about her family history of cancer, as well. Turns out, there were several instances of both breast and ovarian cancer. I knew immediately that this patient was someone who needed genetic testing.
To her credit, the patient quickly agreed, not just out of concern for her own health, but for the health of her daughters and other family members. She was tested, and it was determined that she had the BRCA1 gene mutation, which put her at extensive risk for both breast and uterine cancer. Due to her history with cancer and the discovered gene mutation, the patient decided that after dealing with cancer twice before, she didn’t want to go through it again. She opted for a bilateral mastectomy and bilateral oophorectomy. In the meantime, we tested her daughters for the BRCA1 gene and determined that all three were negative for the mutation.
We continued to follow the patient’s multiple myeloma, but a few years later, her skin suddenly turned yellow. It was soon discovered that she had bile duct cancer, her third malignancy. Once again, the patient underwent surgery, having her bile ducts removed in a Whipple procedure.
After recovering from surgery, the patient came back to undergo chemotherapy at our office. I was astounded. After all she’d been through, she was still smiling. She told me again how grateful she was that her daughters had tested negative for the BRCA1 gene mutation. Her love for her family came across in every word she spoke, and I was proud to have helped set her mind at ease during those difficult times.
This patient has now been living with cancer for more than 30 years. She has a great quality of life, exercises regularly and eats well, and she’s not going to let anything stop her. She’s an inspiration to her family—and frankly, to her doctors. She’s outliving her cancer, and she’s doing it with a smile.

Dr. Eric A. Widra
Obstetrics and Gynecology, Reproductive Endocrinology and Infertility, Shady Grove Fertility
Selecting just one standout patient story is an impossible task. Throughout my career, I have had so many favorite cases that I can’t choose one. I have had cases where a woman donated eggs to her sister so she could start her own family after years of struggle. A family who turned to in vitro fertilization to help them eliminate an inherited disease in their family history. Couples who continually miscarried and were finally able to have a healthy child through IVF and genetic testing of their embryos. The woman whose uterus was lost to cancer or surgery and now has a family by using a gestational carrier. The couple who thought they couldn’t have kids because of a low sperm count. The same-sex couples who need our help to start their families. All of these are a tapestry of favorites whom I have been privileged to help.
Each day, we have a list of patients who have come in for testing, and we review their results in the afternoon. Many of them are having their first pregnancy test after a treatment. As I click on their names, I have the same rush of hope and anticipation for a positive result that I had on my first day as a fertility doctor.

Dr. David S. Yoho
Infectious Disease, Mid-Atlantic Permanente Medical Group, Kaiser Permanente
When an abnormal CT scan showed multiple nodules in the lungs of a patient in 2019, I became very concerned and jumped into action.
I immediately ordered labs to get a more well-rounded idea of her health status. A new diagnosis of AIDS and disseminated tuberculosis was made. The patient was started on four different kinds of TB meds along with steroids and later started on three different kinds of HIV medications. Unfortunately, the patient developed severe immune reconstitution inflammatory syndrome, a known complication after starting life-saving medications. As a result, she developed large areas of swelling and draining abscesses in her neck, which caused her a great deal of distress. Through it all, this patient exemplified great adherence to all forms of the challenging treatment.
In January 2020, four months after receiving the diagnosis of AIDS and TB, the patient’s health took a turn for the worse. Increased swelling in the neck and difficulty breathing led to her admission to a local hospital. The patient underwent an extensive workup during that admission and was found to have B-cell lymphoma, an AIDS-related cancer centered in lymph nodes. The patient sustained nerve damage to her face, tongue and vocal cords, developed a blood clot in the blood vessels of her brain and had a seizure during her first round of chemotherapy, all of which led to an extensive two-month hospitalization. Despite the odds against her, the patient continued to show an unbelievable will to survive. This was an inspiration to me and the other physicians on her treatment team.
Our integrated multispecialty care team immediately engaged to save this patient’s life. Our patient was seen by physicians from neurology, hematology, oncology, neuroradiology and infectious diseases. This coordinated team approach proved to be highly effective. Our patient remains in remission four months after finishing her chemotherapy. She has successfully completed TB treatment and simplified her HIV treatment to one pill once a day, and most importantly, she has her life back.
At every step of her treatment, this patient’s resilience and positive attitude left me in awe. I have no doubt the access to coordinated care saved her life during this pandemic. Her patience and respect for each member of her care team gave us tremendous gratitude for one another and our shared commitment to put our patients first. In midst of a challenging year, she reminded me so many times why I am proud to be a physician with the Permanente Medical Group, where together we always put patient care front and center.

Dr. Ebony R. Hoskins
Gynecologic Oncology, MedStar Washington Hospital Center
This summer, I had an established patient who was diagnosed with a malignant bowel obstruction. She was young, just 41 years old, and admitted in the hospital for four weeks. She wasn’t able to eat or drink, and she was in significant amounts of pain. There came a point in her hospital stay when I questioned myself, “Will she leave the hospital alive?” I think what made her hospital stay even more difficult was the fact that she couldn’t have any visitors. I did not realize visits from family and friends were such a critical component in the healing process prior to the onset of the global pandemic. Four weeks may not sound like a long time, but in a hospital, without visitors, it can feel like a lifetime. The doctors, nurses and staff attempted to fill that void, but it’s just not the same. We are able to take care of patients medically and surgically, but there is a strong component of family support that is needed to help them emotionally, mentally and spiritually. It’s been difficult during the COVID pandemic because medical providers and staff cannot provide all of those essential components, as much as we would like to.
Thankfully, she turned the corner and was able to leave the hospital eating and drinking. Fast forward to six months later: She’s completed her chemotherapy plan, and her recent imaging shows no evidence of disease. She is doing well physically, emotionally and spiritually.
This experience with my patient showed me as a doctor that medicine is not the only component needed for healing. My patient was a woman of faith, and there really is a mind, body and spirit connection that contributes to the healing process. We get to the point in medicine where we can do everything in our power—use the best medicine, have access to the best resources—but there’s also an element to the human body where the spirit helps to heal.
Recently, I got the COVID-19 vaccine, and I’m hopeful that cancer patients and the general population are willing to get inoculated as soon as it becomes available. This will give us more normalcy and hopefully will allow visitors back into the hospital. Prior to the global pandemic, it was easier to take visitors for granted. Now we know just how important family and friends are in the healing process.

Dr. Richard F. Neville
Vascular Surgery, Inova
For my entire career, helping my patients save their limbs has been a passion. I have been dedicated to restoring circulation to promote healing and avoid amputation. Unfortunately, amputation remains a significant problem in our health care system and around the world, so much so that some of my colleagues and I started a society—the Critical Limb Ischemia Global Society—to address the issue. The problem is that when someone has an amputation, it’s more than just losing the limb. Patients have a very high incidence of having the other leg amputated in a couple years and an increased mortality rate. So I always tell people that we’re not only saving your leg, but also keeping you functional and, in many ways, expanding your life span. We are currently building a multidisciplinary team at Inova to focus on limb preservation, including advanced vascular techniques as well as state-of-the-art podiatric and plastic surgical care.
Even as we work on this issue, the number of amputations being performed in America remains significant, in large measure because diabetes is skyrocketing, and diabetes can lead to amputation. Coupled with that, there’s a disparity of care delivery that impacts amputations. This disparity seems to inordinately impact some of our less fortunate socioeconomic populations. Low-income Hispanic and African American populations have a higher incidence of being initially treated with amputation versus attempts at limb healing and preservation.
As a surgeon interested in education and research, I have always believed it’s important to advance techniques and improve outcomes. But I am also strongly motivated in this field by connecting with my patients—striving to not only save their limbs but to also make sure they can remain independent and maintain their quality of life. Recently, I had a patient, a 75-year-old woman from Jamaica. She has diabetes and had already had other vascular treatments, including angioplasty, by the time she came to my office. She had been told nothing else could be done and she needed to undergo leg amputations. We were able to perform successful bypasses on both her legs, and just recently she was in my office for a follow-up. With tears in her eyes, she told me that because we saved her legs, she’d be able to go to Jamaica for a 50th anniversary family reunion, and that just meant so much to her. And it meant so much to me, too. Not only did we save her limb, but that also means she gets to stay mobile, live by herself and be independent. I’ve done thousands of surgeries at this point in my career, and while I love the technical aspect of it, it’s stories of patients like her that I live for.

Dr. Perry K. Richardson
Neurology, The GW Medical Faculty Associates
Neurology and the healing arts conjoin in unexpected ways. Imagine my surprise when I entered the exam room to find a patient and his guitar. Mine was the first formal neurological consultation, though a different neurologist astutely noticed the dystonia that rendered his dominant hand almost useless.
His recital was my examination. I watched his fingers splay and wobble as he attempted to play notes, sabotaged by a bedeviling programming glitch in his brain.
His malady, focal dystonia, has disabled writers, musicians, athletes and others. It is the cause of writer’s cramp, which for years was thought to be a psychological condition, akin to “writer’s block.” This prejudice was countered by the official designation “organic writer’s cramp,” after researchers found involuntary co-contraction of competing muscles as its basis.
He was a TV celebrity and composer in his home country for years, delighting audiences with his “baladas romanticas.” Bolero sprung from his skilled hands after practicing assiduously to perfect runs up and down the fingerboard. He emulated Luiz Bonfá and Baden Powell. Then, playing, writing and typing were hobbled for 30 years by what doctors called arthritis. But there was no pill, no exercise, no counseling for this plight. It manifested at first exclusively and eerily only while playing guitar. It was as if the constant repetition and intricacy of fingering stymied and then short-circuited the neurons responsible for the proper execution of hand use. Unfair in its harshness, it later impaired even daily manual tasks like writing and buttoning.
We chatted about our musical heroes, Tom Jobim, João Gilberto and Celia Cruz (“¡Azúcar!”), as I planned out the target muscles for the treatment: injections of botulinum toxin, one of the strongest poisons on the planet. The goal was to relax the unwanted spasms so that the movement sequences could allow his musical ideas to bloom. Music, his upended lifelong passion, was restored, precision returning to his fingers.
I am often moved by the role I play in people’s lives. I feel immense reward in helping untangle neural knots. In this case I feel I helped bring back two entities—the craft of his hand and the purpose of his trusted guitar.
This story originally ran in our February issue. For more stories like this, subscribe to our monthly magazine.