Hospitals across Northern Virginia are embracing technologies and programs that improve the odds for patients and take the hassle out of health care in the process.
By Sarah Markel
Living in the shadow of the nation’s capitol, it’s easy to overlook the resources available right in our own backyard. Just in the past year, however, seven of Northern Virginia’s hospitals began offering medical approaches and technologies that equal, or even improve upon, those of the nation’s major teaching hospitals.
Access to care is increasing. Outcomes are improving. Best of all, these resources are available without having to travel far from home.
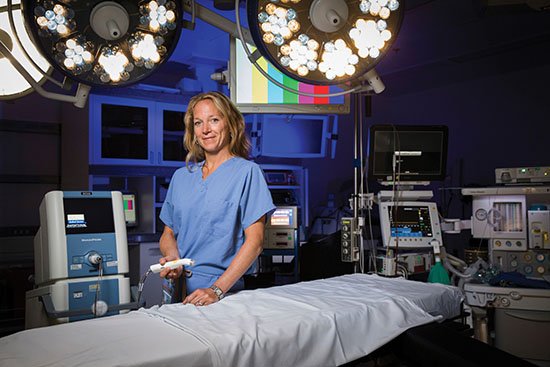
Simple Device Takes Breast Surgery Beyond the Margins
As if a breast cancer diagnosis weren’t bad enough, most patients must endure several anxious days after a lumpectomy to find out whether their surgeon was able to remove all of the cancerous tissue.
Because cancerous breast tissue—especially microscopic tissue—looks just like healthy tissue, it is difficult for breast surgeons to be sure they removed all of a tumor. “Most of time when you can’t tell the difference,” explains Dr. Stephanie Akbari, medical director of the Reinsch Pierce Family Center for Breast Health at Virginia Hospital Center.
That’s why, about 40 percent of patients nationwide end up going back for a second surgery. But not at Virginia Hospital Center. There, thanks in part to a recently-approved device called the MarginProbe, Akbari and Dr. Molly Sebastian have reduced their second surgery rate to five percent.
They use the MarginProbe during surgery to test the surface of a tumor for cancer cells. Akbari explains the goal is to remove a margin of healthy tissue along with the tumor. Because the MarginProbe gives real time information, they can continue to remove tissue until they get a clear margin.

“It’s pretty self-evident why this is a breakthrough,” says Akbari, who also took part in the FDA trial of the device. Initially she had reservations that the device might cause surgeons to remove more tissue than necessary. In practice, she has found it enables her to be more strategic in her work. “It allows me to do smaller lumpectomies because I know I have a back up there to check.”
The MarginProbe has not been widely adopted because it is not yet covered by most insurance plans. However, every patient who comes to Virginia Hospital Center for a lumpectomy benefits from the MarginProbe. The hospital absorbs all expenses associated with the $1,000 disposable device.
Adrian Stanton, vice-president of Virginia Hospital Center says the hospital does this because it’s the right thing to do. Akbari puts it another way: “We use all the tools available in 2014 to make sure that patients won’t need a second surgery for the same cancer.” • The Reinsch Pierce Family Center for Breast Health at Virginia Hospital Center, 1625 N. George Mason Drive, Suite 315, Arlington; centerforbreasthealth.com
New Hope for Patients with Difficult-to-treat Cardiac Conditions
Cardiac care has come along way in recent decades. Until recently, for one group of patients—those with coronary atherosclerosis—there have been few good treatment options, even at leading cardiac care centers.
When the arteries that supply blood to the heart become hardened and narrowed by a build up of plaque on their inner walls, less blood can flow through them. The heart does not get the oxygen it needs. This can lead to chest pain or a heart attack.
The standard treatment is to insert a stent or a balloon in the artery to increase blood flow. But as Dr. Bryan Raybuck, medical director of the Cardiac Catheterization Laboratories at the Heart and Vascular Institute at Inova, Fairfax, points out, about
10 percent of patients with this condition have severe calcification in the plaque, which makes it hard to expand the balloon or stent.
Now, with the help of a recently approved device called the Diamondback 360 Coronary Orbital Atherectomy System, surgeons at Inova Fairfax Hospital are safely and effectively treating those patients without the need for bypass surgery. Inova is the only hospital system in the mid-Atlantic region to adopt this technology and train their surgeons to use it.
Using the Diamondback 360, surgeons access the arteries through a patient’s wrist and gently sand away the calcified plaque lesions. This enables them to successfully place a balloon or stent.
“This is the first advancement in this field in 20 years,” says Dr. Shawn Yazdani, an interventional cardiologist with Carient Heart & Vascular Institute. “It’s allowing us to tackle the lesions where before the patient would have required cardiac surgery.”
The minimally invasive procedure—20 minutes versus a few hours of open-heart surgery—vastly reduces the rate of complications, such as bleeding, and the chance a second operation will be needed later.
Mary Obannon, 80, was one of the first patients to benefit from the Diamond Back 360. After a heart attack in May, Obannon, who lives in Marshall, was transferred from her community hospital to Inova Fairfax. There Yazdani used the Diamondback 360 to place a stent in a heavily calcified artery near her heart. “Honestly, I was shocked,” says Obannon, who returned home the following day. “It didn’t even hurt.”
Raybuck estimates that eventually the device will provide an ideal treatment option for about 200 patients a year. “These are the toughest cases,” he says.
The Diamondback 360 is just one of many new technologies that keeps Inova on the cutting-edge of cardiac care. Other examples include a minimally invasive valve replacement procedure and a technique that opens blocked arteries without open-heart surgery. Inova also participates in clinical trials, most recently one examining the safety and efficacy of bioabsorbable stents. • Inova Heart & Vascular Institute at Inova Fairfax Hospital, 3300 Gallows Road, Falls Church; inovaheart.org

Smart Medicine Gets Personal
Under the current model of medicine, doctors try one treatment and then another until something works. This approach takes time. It’s costly. And it’s not always effective. Researchers at the Inova Translational Medicine Institute (ITMI) have an alternative approach. They are using genomic sequencing to develop a new paradigm of medical care—one that uses genetic information to predict who will get sick and to develop personalized treatment plans for each individual.
A decade ago, when Whole Genome Sequencing (WGS) was introduced, the cost of sequencing an entire human genome—some 21,200 genes—was exorbitant, approximately $100 million for the first sequence. Now it’s a few thousand dollars per genome. The data revealed by a simple blood test allows scientists to look for disease-causing genetic alterations that could put a person at risk for certain disorders such as cancer, diabetes and cardiovascular disease. It can also reveal if a person has inherited genetic disorders such as a genetic immunodeficiency.
“The challenge is how [to] make this kind of information usable for a physician at the point of care in real time,” says Dr. John Niederhuber, executive vice president of Inova Health System and CEO of ITMI.

Answering that challenge is what makes the work of ITMI distinctive. Even though the institute is privately funded and staffed by physicians, scientists, statisticians and bioinformaticians—the people who develop algorithms for analyzing biological data—it operates within the setting of a suburban hospital. As advances are made, area patients will benefit.
Some of the studies currently underway at ITMI are investigating diabetes, asthma and treatments for patients with heart failure. However, ITMI’s three largest studies all focus on studying the genetic sequence of what is known as the family trio—mother, father and infant. “The goal of this research is to try to understand factors related to early childhood health, as well as related health issues,” says Dr. Benjamin Solomon, chief of the division of medical genomics at ITMI.
One of these studies identifies babies in the the neonatal intensive care unit (NICU) whom doctors suspect could have a genetic disorder because of medical conditions that cannot be attributed to any other cause. Already 80 families have taken part in that study; ITMI researchers have closely analyzed the genetic codes of seven babies.
“In many of those cases, we’re finding information that should be very helpful,” says Solomon. In one case, genetic testing revealed compromised adrenal function in a child scheduled for surgery. “Pinpointing that molecular change altered the medical care this child received during surgery,” Solomon says.
As Niederhuber notes, the ability to tailor medications to the individual is just the first of many ways in which genomics will transform health care over time: “We believe the future of medicine is to learn as much as we can about an individual as early in life as we can and to prevent diseases from occurring.” • Inova Translational Medicine Institute, Claude Moore Building, 2nd Floor, 3300 Gallows Road, Falls Church; inova.org
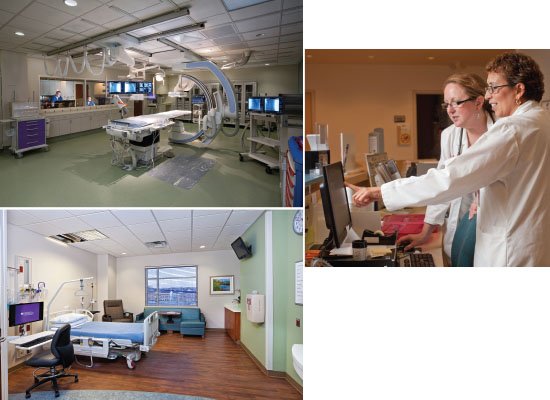
New Hospital Blends World-Class Health Care with Small Town Convenience
Residents of Haymarket no longer have to battle a half hour or more of traffic to access health care since the opening of a new 60-bed hospital, Novant Health Haymarket Medical Center, in March. It joins Prince William Medical Center as the second Novant hospital in the region. The two hospitals work in tandem to meet the needs of their respective communities. “Our physicians practice at both facilities,” says Melissa Robson, president of Novant Health Northern Virginia. “There are unique differences at each facility in terms of specialties offered.”
Novant redistributed some of its beds and services to meet the needs of the Haymarket community. The cardiac services and NICU have remained in Manassas, while an innovative breast care center and a weight management program are planned for Haymarket. The new hospital was designed with input from patients, care providers and families at the Manassas hospital.
Gainesville resident Don Brown, 79, thought he was having a heart attack one morning shortly after the hospital opened in March. During a previous heart attack, it took 30 minutes for him to reach the nearest hospital by ambulance. This time, he jumped in his truck and drove himself the few miles to Haymarket. “I thought I could get here faster than an ambulance,” he jokes. “It’s wonderful having something that close.”
Besides convenience, the new design offers many patient-focused design features: spacious, square-sized patient rooms; in-room storage closets with all supplies and equipment within reach; in-room computers to update patient records; showers in the critical care unit; and sofa beds that convert to dining tables, taking the comfort of visiting family members and guests into account.
Robson says this is just the beginning. The fourth floor of the hospital has yet to be completed. “We are looking to evolve over time based on the needs of our community.” • Novant Health Haymarket Medical Center, 15225 Heathcote Blvd., Haymarket; novanthealth.org
Nurse Navigators Provide Comprehensive Joint Replacement Experience
Surgery is stressful enough. When knee, hip or shoulder replacement is part of the picture, uncertainties about insurance approvals, the actual hospital stay, wound care and the prospect of grueling hours of physical therapy can compound that stress. Sentara Northern Virginia Medical Center in Woodbridge launched a program this spring that makes the entire joint replacement process easier for patients.
It starts with a phone call from Ada Vega-Diamantis, the orthopedic nurse navigator at the Sentara OrthoJoint Center. She invites patients to tour the hospital and attend a pre-surgery class. “One of the therapists from rehab attends the class as well as [a] member of the care coordination team,” Vega-Diamantis explains. “We discuss our expectations, their expectations and the routine of the procedure.”
The class also functions as a de facto support group. Patients make connections that last through rehab and beyond. Vega-Diamantis says joint replacement is no longer limited to seniors. Many of her patients are in their 40s and 50s.
After the class, Vega-Diamantis follows up with phone calls and text messages to ensure patients have forms and pre-operative lab work completed. After surgery, she is back at each patient’s bedside, giving wound care advice and coordinating with surgeons, physicians and physical therapists.
Already anecdotal evidence suggests the program is reducing the number of patients who visit the emergency department for post-operative complications. The OrthoJoint Center also benefits the community by providing high levels of care so patients do not have to travel far for treatment. • Sentara Northern Virginia Medical Center, 2300 Opitz Blvd., Woodbridge; sentara.com
House Calls From the Emergency Room
Single parents in the middle of the night; office workers on a coffee break; a guy sitting in a booth at McDonald’s. Dr. Dennis Truong, an emergency room physician for Mid-Atlantic Kaiser Permanente has seen them all. But, he hasn’t actually met them.
Dr. Truong is the lead physician for Kaiser Permanente’s new House Calls program, a video chat initiative that allows patients with any one of 22 minor ailments to receive treatment from the convenience of their homes, offices—or anywhere else—24 hours a day.
“Telemedicine is nothing new,” explains Truong. This program is unique because it is managed out of the hospital’s call center. To callers who fit certain profiles, operators offer the caller the option of in-person appointment, a call from the advice nurse or a video consult with one of several board-certified emergency physicians.
“We have set up scripts and protocols to make sure it [is] a safe option,” explains Truong. He points out that telemedicine is perfect for complaints such as colds, urinary tract infections and rashes.
The HouseCalls doctors have access to Kaiser Permenente patient records. They can make appointments, send prescriptions to the pharmacy and order lab work. About 20 patients a day choose the telemedicine option. Some HouseCalls consults turn out to require in-person intervention. In those cases, patients are referred to the emergency room or scheduled to see a specialist.
The program is available at no cost to patients. Kaiser Permenente views it as a patient satisfaction tool. And it increases efficiency. “The HouseCalls program helps the hospital function in general because it gets our patients to the right places,” says Dr. Truong. • Multiple locations; kp.kaiserpermanente.org
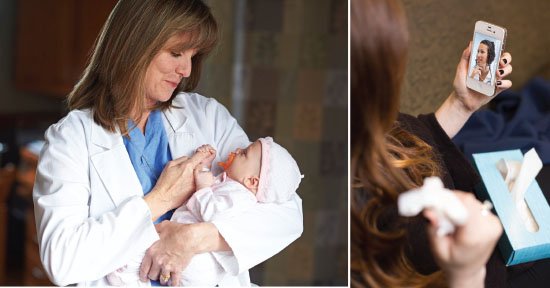
Telemedicine Delivers Advanced Infant Care to Rural Communities
Babies born at Fauquier Hospital in Warrenton now have immediate access to advanced neonatal care through an innovative telemedicine program with the University of Virginia Health System (UVA). This is first neonatal telemedicine program in Virginia. It ensures that newborns with complications have immediate access to neonatal specialists without having to travel far from home.
The relationship between Fauquier and UVA is not new. As Maria Juanpere, M.D., medical director of nursery and pediatrics at Fauquier Hospital explains, “Our hospital has always had a collaborative relationship with UVA—it’s gotten stronger as new technology has come out.”
Previously, nurses and physicians at Fauquier Hospital’s Family Birthing Center spoke via telephone with neonatologists at UVA’s NICU. They described the infant’s condition while looking at a medical record. Now a high-resolution video camera attached to a rolling cart allows Fauquier’s medical team to meet with UVA neonatologists right at the crib of a sick baby. Together they look at the infant, discuss possible diagnoses and develop a treatment plan. “It’s very helpful when there is something visibly different with the baby,” explains Dr. Juanpere, who points out that many neonatal skin conditions can have two or three possible diagnoses.
“This technology helps us develop a working diagnosis so we can treat that baby appropriately,” she says. The telemedicine program also helps UVA neonatologists quickly determine which infants need to be transferred to UVA’s 45-bed NICU and which ones can be safely cared for at Fauquier.
Meanwhile, the nurse practitioners and physicians at Fauquier are expanding their treatment capabilities so that fewer infants will require transfer to UVA. • Fauquier Health, 500 Hospital Drive, Warrenton; fauquierhealth.org
(August 2014)




